This section covers:
- The uses of epidemiology and other methods in defining health service needs and in policy development
- Formulation and interpretation of measures of utilisation and performance
Health needs assessment (HNA) is an essential tool to inform commissioning and service planning, and can be defined as a systematic method of identifying the unmet health and healthcare needs of a population, and making changes to meet those unmet needs. HNA allows for appropriate targeting of resources, and often involves working in partnership with other agencies, communities and service users. Indeed, HNA can be an excellent opportunity to involve stakeholders in service planning and increase ownership and sustainability. HNA may focus on specific diseases, population groups, procedures or interventions.
CONTENT
- Need, demand and use
- Defining Health Needs Assessment
- Approaches to Health Needs Assessment
- A Health Needs Assessment Framework
1. NEED, DEMAND AND USE
Need
The term need is used by a range of both health and non-health professionals in different and varying contexts. Jonathon Bradshaw defines four ways in which need is perceived:
- Normative need, based on professional judgement (such as the need for medical treatment)
- Felt need, which comprises individual's perceptions of variations from normal health
- Expressed need, which can be the vocalisation of need or how people use services
- Comparative need, based on judgements by professionals as to the relative needs of different groups
Bradshaw's typology does not, however, include any analysis of clinical or cost-effectiveness. Many health economists, therefore, use the population's ability to benefit from health care interventions as a working definition of need. It is important to distinguish between the need for health, and the need for health care. The former term includes health problems where there is no realistic or available treatment, and which do not inform the planning of health care services (The epidemiological approach to health care needs assessment. Stevens A, Raftery J, Mant J. www.birmingham.ac.uk/.../college.../Health-care-needs-assessment.pdf). For the purposes of health needs assessment, need is assumed to exist when there is an effective and acceptable intervention, or the potential for health gain. The ability to benefit from health care can be influenced by several factors including the epidemiology of the disease and the effectiveness of interventions (Need for redefining needs. Asadi-Lari M, Packham C, Gray D. Health and Quality of Life Outcomes 2003, 1:34). Therefore, a comprehensive needs assessment should also include an assessment of evidence of effectiveness. Need should also be distinguished from demand and use.
Demand
Broadly speaking, demand for health care services is the expression of felt need, i.e. the services that people ask for. Demand is influenced by a range of factors including:
- Illness behaviour (itself influenced by age, gender, education, socioeconomic class)
- Knowledge of services
- Influences from the media.
Demand is also influenced by the supply of services, which is itself influenced by the use of guidelines, and evidence of clinical and cost-effectiveness. As with the laws of supply and demand, demand for health care increases with supply or accessibility, making demand a generally poor proxy for need. Need, supply and demand all overlap to a degree (Figure 1).
Figure 1: Need, supply and demand
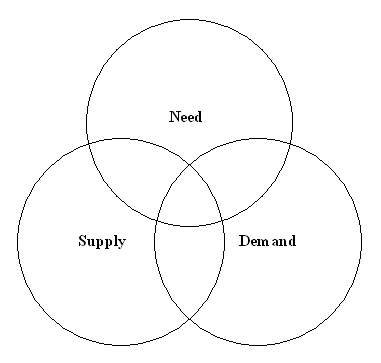
Use
Service utilisation may be measured in different ways, for example by:
- Service-based activity, such as GP referral rates, bed occupancy, intervention rates
- Population-based activity such as prescriptions, immunisation coverage, surgical rates
Variations in utilisation may be due to a number of factors including:
- Statistical factors (incomplete data, bias, etc)
- Demand factors (age/sex composition, morbidity rate, illness behaviour)
- Supply factors (availability of services, professional judgement); which are usually the main reason for variation in use of services.
Julian Tudor Hart describes the relationship between need, use and availability of services in the inverse care law, which states “the availability of good medical care tends to vary inversely with the need for it in the population served. This ... operates more completely where medical care is most exposed to market forces, and less to where such exposure is reduced." (Tudor Hart, 1971).
2. DEFINING HEALTH NEEDS ASSESSMENT
The World Health Organisation describes health as “a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity." Health and wellbeing are the consequence of a wide range of factors, summarised in the rainbow model from Dahlgren and Whitehead.
Figure 1 The Dahlgren and Whitehead model
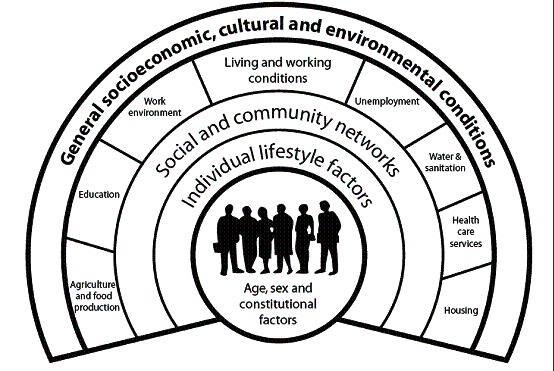
The statutory duty of Joint Strategic Needs Assessment, which will be undertaken by local authorities and clinical commissioning groups (CCGs), through the health and wellbeing board, is an opportunity to examine these wider determinants of health as part of a broad assessment of local needs.
3. APPROACHES TO HNA
Stevens and Raftery describe three approaches to HNA.
- Epidemiological. This approach considers the epidemiology of the condition, current service provision, and the effectiveness and cost-effectiveness of interventions and services.
- Comparative. This approach compares service provision between different populations. Large variations in service use may be influenced by a number of factors, and not just differing needs.
- Corporate. This approach is based on eliciting the views of stakeholders - which may include professionals, patients and service-users, the public and politicians - on what services are needed. Elements of the corporate approach (i.e. community engagement and user involvement) are important in informing local policy.
From: The epidemiological approach to health care needs assessment. Andrew Stevens, James Raftery, Jonathan Mant. www.birmingham.ac.uk/.../college.../Health-care-needs-assessment.pdf In practical terms, HNA often incorporates elements of all three approaches.
4. FRAMEWORK FOR UNDERTAKING HNA
HNA involves gathering information to inform service planning with the aim of improving health. Services may need to change for a number of reasons, including:
- Inequalities in outcomes
- Local sensitivities
- Changing demographic patterns or disease trends
- Availability of new treatments
- Changing expectations
Ensuring the commitment of senior managers to the HNA is most likely to ensure implementation of the recommendations. There is no single approach to undertaking a health needs assessment, and the approach used may vary according to local circumstance including available time and resources. Health Needs Assessment: A Practical Guide identifies a number of steps or stages (below). Whilst these are presented in a sequential manner, many of these stages overlap or can be carried out in parallel.
The five (modified) steps are:
Step 1: Getting started
HNA is often a multidisciplinary task. Early stakeholder involvement is crucial in identifying who will carry out which elements of the assessment, and ensuring engagement of all parties. This stage should include:
- Identifying the population of interest - is it defined by geography, illness, social experience (i.e. asylum seekers, homeless people, etc) or setting (for example, prison or school)?
- Identifying the key stakeholders
- Identifying what resources are available
Step 2: Identify health priorities
- This stage involves gathering data describing the population of interest. This may involve collection of both quantitative and qualitative data, which are then analysed to give a detailed picture of health needs. This stage may involve collecting data on similar localities to allow comparisons of need.
- This stage should also incorporate a review of current levels of service provision, which may include information on infrastructure and workforce/skills
- Assess evidence of effectiveness
Step 3: Identify priorities for change. This stage should identify which of the issues identified are most important, leading to priorities for action. Priorities may be decided on the basis of:
- Size and severity impact
- Availability of effective and acceptable interventions and actions
- Local commissioning priorities and partnership arrangements
Steps 4 and 5:
- These steps involve implementing the changes, developing a monitoring and evaluation strategy, and measuring the impact of the changes in services.
© Dr Renu Bindra 2008, Claire Currie 2016
