Professional Accountability in the NHS
This section covers:
- Professional accountability - clinical governance, performance and appraisal
The term accountability has been described as,
the obligation of one party to provide a justification and to be held responsible for its actions by another interested party
Accountability is a complex phenomenon and It is therefore helpful to view it is as having three components:
- The individuals professional accountability for the quality of his or her own work.
- The accountability of health professionals within the organisations in which they work.
- Accountability (with others), as a senior member of staff, for the organisations performance and more widely for its provision of local services.
For the first 40 years of the National Health Service the accountability of doctors was to their patients and to a broad and non-specific professional code. To begin with the NHS provided a setting where doctors could exercise their skills with almost complete autonomy. However, the advent of managed care in the 1980s followed by the acknowledgement of the rights of service users in the 1990s led to the production of evidence based guidelines for an increasing number of diseases and patient groups. By the new millennium the obligation was placed on clinicians to meet some explicit and higher professional standards. All these changes have highlighted the duty of clinicians to continuously strive to develop professionally - to acquire and retain clinical skills, to access and use best evidence, to participate in planning for quality, and to evaluate and optimise processes of care. These new and explicit forms of accountability have been captured in the concept of clinical governance.
Clinical Governance
The term clinical governance became prominent following the publication of New Labours first White Paper on health, The New NHS: Modern, Dependable (1997) and subsequently Quality in the New NHS (1998). This modernising agenda focused on quality improvements, with clinical quality a key focus, placing duties and expectation on local health-care organisations as well as individuals (DH 1997:34) to provide clinical excellence. Clinical Governance is the vehicle put in place to tackle the wide differences in the quality of care throughout the country. In the past it has been difficult to produce a universally accepted definition of clinical quality, the government has attempted to do this through the idea of clinical governance:
Clinical governance is a framework through which NHS organisations are accountable for continuously improving the quality of their services and safeguarding high standards of care, by creating an environment in which clinical excellence will flourish (DH 2009)
In 1997, six principles of clinical governance were described in making the NHS modern and dependable:
- To re-establish the NHS as a national service for all patients throughout the country, where patients will receive high quality care regardless of age, gender or culture if they are ill or injured.
- To establish national standards based upon best practices, which will be influenced and delivered locally by the healthcare professionals themselves, taking into account the needs of the local population.
- Collaborative working partnerships between hospitals, community services and local authorities, where the patient is the central focus.
- To ensure that the healthcare services are delivering high quality care and providing value for money.
- To establish an internal culture where clinical quality is guaranteed for all patients.
- To enhance public confidence in the NHS (DH 1997).
In June 1998, the Government published proposals to put quality "at the heart of
healthcare" (A first class Service Quality in the new NHS 1998). There are three components to the strategy: setting clear standards, developing local systems for achieving them, and monitoring whether this has been achieved. The links between the three are illustrated below.
|
Standards set by: |
Standards delivered locally through: |
Standards monitored by: |
|
National Institute for Clinical Excellence (NICE) |
Professional self-regulation |
Commission for Health Improvement (CHI) |
|
National Service Frameworks (NSFs) |
Clinical Governance |
National Performance Framework |
|
Lifelong learning |
National Patient and User Survey |
These concepts of clinical governance are underpinned by a statutory Duty of Quality introduced in the Health Act of 1999. There are a range of contributing factors for introducing clinical governance within the NHS, some of which have been identified through the following political, public and professional demands:
The drivers of clinical governance (after McSherry & Pearce 2007)
|
Political |
Public |
Professional |
|
Changes in health policy: Uncontrollable expenditure to meet rising public demand The resulting focus on organisational, managerial and financial aspects (Griffiths Report 1983) Development of market forces and the purchaser / provider split (Working for Patients 1989) Strong emphasis on achieving clinical quality (The New NHS: Modern, Dependable 1997 & Quality in the New NHS 1998). |
Rising patient and public expectations and involvement: Patients as consumers of healthcare (The Patients Charter 1992) Individuals becoming active in the delivery of health services (The Citizens Charter 1993) |
Increased patient dependency: Rising number of elderly people with complex physical and social problems Advances in stroke care and rehabilitation The need for greater efficiency reduction in length of hospital stay |
|
Demographic Changes: Increase in life expectancy and changes in morbidity & mortality (Health of the Nation 1991) Focus on health promotion and disease prevention Widening inequalities in health, wealth and disease |
Advances in healthcare technology: Supported the quality and standards of nursing care delivery Need for training in safe equipment usage for staff and independent contractors |
|
|
The impact of organisational change on the provision and delivery of healthcare: Increase in number of patients admitted with multiple needs Development of services to maintain individuals in the community Reduction in junior doctors hours increase in nurse consultants and therapists Increase in life expectancy with greater healthcare needs |
Lack of public confidence in healthcare provision: Media publication of clinical succeses and failures e.g. Bristol Royal Infirmary (1998) |
Rising number of complaints going to litigation: Huge rise in formal complaints made by pateints and careres about hospital and community services Many instances of complaints arising through system failures rather than actions or omissions of individuals Need to develop a fair blame culture with open reporting dicussion and learning from clinical incidents or clinical complaints |
|
Trend towards greater access to healthcare information: Advances in IT and internet resulting in easier access to information by the public The Cochrane Library and DH website inform patients about specific conditions Rising expectations from patients |
The key to clinical governance is trust; individuals and teams must be able to trust the orhanisational systems I which they work, confident that other individuals and teams are making their stated contribution to patient care. Clinical governance cannot be successfully implemented without the support of the non-clinical aspects of healthcare delivery. Healthcare provision and delivery is complex in nature and relies upon good teamwork, effective leadership and sound management. Organisations and individuals are therefore required to embrace the concept of clinical governance in the pursuit of clinical excellence as a journey. The big opportunity offered by clinical governance is the opportunity to change systems to pull together different components and strands from the clinical and managerial worlds to improve things for patients. These components need to be available and achievable throughout the organisation. A healthcare organisation that is innovative, involving staff from all levels of the organisation and patients/carers, is an ideal foundation for the implementation of clinical governance.
The most recent, Next Stage Reviews High quality care for all (2008) says, Enabling all parts of the NHS to focus consistently and systematically on improving the quality of care is a major challenge. It requires a long-term transformation that touches all parts of the system, starting from the front line.
Performance
Definitionsof clinical governance have emphasised the responsibilitiesof individuals, highlighting the importance of lifelong learningby all clinicians and creating a clear obligation tomanage poor professional performance when it is identified.
NHS performance has improved dramatically since 1997 with shorter waiting times, improved access to primary and secondary care, reductions in deaths from cancer and circulatory disease and significant reductions of hospital associated infections have all been delivered in the last twelve years. The results of the 2007/08 Healthcare Commission Annual Health Check confirmed that the NHS is both delivering a better quality of service and using the resources it has more effectively.
To deal with poor performance, clinical governance leaders need skills to assess the nature of the problem, educational resources to deal with it, and managerial resources to facilitate the process. The Department of Health has introduced a new NHS Performance Framework to provide a dynamic assessment of the performance of NHS providers (that are not yet NHS Foundation Trusts) and commissioners against minimum standards. Effective regulation remains a key aspect of the Departments drive to make quality the organising principle of the NHS and the Performance Framework complements the work of the regulators. It has been co-produced with stakeholders from across the NHS, the NHS Confederation, Monitor, and the Care Quality Commission. The consistency and transparency afforded by the Performance Framework will better enable all parts of the system to work together to tackle underperformance. The Performance Framework creates a single definition of success against which NHS organisations will be judged. Five overarching principles that govern the development of the NHS Performance Framework to ensure that it is:
Transparent: with clear and pre-determined performance measures and interventions
Consistent: having a uniform approach across England, at different levels of the system, and across different types of providers
Proactive: with thresholds for intervention that identify underperformance at an early stage so that it can be addressed swiftly
Proportionate: intervention will be related to risk, for example, problems at service level will be addressed through interventions at service level
Focused on recovery: initial interventions will focus on recovery and will include action to address the root causes of issues, including system-level risk such as over-capacity. The NHS Performance Framework has also been developed in accordance with the Departments principles for change.
The Framework sets clear thresholds for intervention in underperforming organisations and a rules-based process for escalation, including defined timescales for demonstrating improved performance. Organisational performance will be assessed against a series of indicators using the most current data available, and the results will trigger intervention by SHAs and PCT commissioners in the case of performance concerns. Performance will be assessed across four key domains of organisational function:
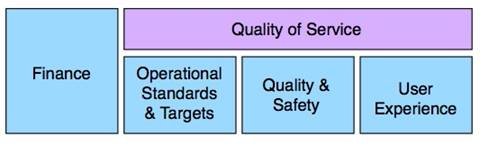
(DH 2009:12)
Quality is at the heart of the NHS Performance Framework: User Experience clearly measures the experience of patients, while Quality and Safety, and Operational Standards and Targets relate to both patient safety and effectiveness of care. Each domain is underpinned by a series of indicators, largely from existing sources, and a scoring system to determine performance thresholds. Where there is currently no data, the Department will continue to work with key stakeholders to develop indicators to assess performance. The domains of organisational performance that will be measured as part of the framework span managerial and clinical priorities and have the buy-in of clinicians and managers alike.
The following table articulates how the Performance Framework combines national transparency and consistency, with a degree of local flexibility:
|
Nationally the framework has determined |
|
|
What is assessed |
Measuring performance through national indicators |
|
When performance concerns are identified |
Identifying performance concerns through the appropriate use of thresholds and on a quarterly basis |
|
Locally the framework allows discretion in |
|
|
How organisations with performance concerns are supported |
SHAs and PCT commissioners will be responsible for determining the nature of the remedial intervention aimed at supporting recovery |
(DH 2009:11)
The Care Quality Commission (CQC) has a vital role in providing assurance that all health and adult social care services meet essential levels of quality and safety, and will contribute to the wider drive for ongoing service improvement. While Monitor, as the independent regulator of NHS Foundation Trusts (FTs), will continue to ensure that FTs comply with the terms of authorisation that set out their obligations on financial and service performance and governance. An illustration of how we may be able to achieve these requirements of coherence in developing a performance framework for PCTs and NHS Trusts is described in the table below.
Ensuring coherence in performance assessment across the system
(DH 2008b:38)
|
Domain |
Domain Possible approach to performance assessment |
|
|
Finance |
Financial metrics For NHS Trusts the metrics would be based on Monitors financial risk assessment used for Foundation Trusts, adjusted to reflect their statutory duties and the requirements of the Operating Framework. For PCTs, the starting point would also be a Monitor style of risk assessment, with further metrics developed to recognise the commissioning role of the PCTs, statutory duties and the requirements of the Operating Framework. |
|
|
Service performance |
Operational Standards and Targets |
Vital Signs, including Tier 1 indicators (i.e. national requirements) and existing operational standards |
|
Quality and Safety |
Compliance with minimum requirements of quality and safety or registration requirements (ie. a development of the core standards that underpin the current role of the Healthcare Commission) Performance against clinical indicators (TBD) |
|
|
User Experience |
Vital Signs indicators, based on survey results |
|
|
Board Capability |
For PCTs, outputs from the annual commissioner assurance process. For NHS Trusts, outputs from the FT diagnostic, refreshed on a risk basis, according to evidence of underperformance in other domains. |
|
A national performance dashboard incorporating indicators from the Vital Signs, introduced under the 2008/09 Operating Framework, support local target setting and performance monitoring against both national and local priorities. The Vital Signs incorporate relevant components of the National Indicator Set (NIS) for local authorities. The Vital Signs include indicators of overall health and health inequalities (i.e. health outcomes); performance against operational standards and targets; and user experience.
For an example of a perfomance dashboard (see http://ww2.swindon.gov.uk/moderngov/)
Appraisal
The drive for a formal Appraisal process for all doctors in the NHS came from the introduction of the concept of Clinical Governance outlined in the 1998 consultation document A First Class Service Quality in the New NHS. The primary aim of NHS appraisal is to identify personal and professional development needs. This exercise is different for consultants, non-consultant career grade doctors, and GPs. Appraisal is an important contribution to the quality agenda, it offers a forum in which good work can be recognised, strengths acknowledged and built on, and problems identified and tackled. The appraisal should be a formative,professionally led review of strengths and weaknesses rather thana punitive managerial process.
In 1999, the General Medical Council (GMC), stated that in order to maintain their registration, all doctors must be able to demonstrate that they can continue to be fit to practice in their chosen field. Appraisal is based on the GMCs document Good Medical Practice (General Medical Council, 2001, updated 2006), which describes the principles of good medical practice, and standards of competence, care and conduct expected of doctors in all aspects of their professional work. These are:
- Good clinical care
- Maintaining good medical practice
- Teaching and training
- Relationships with patients
- Working with colleagues
- Probity
- Health
All doctors will be required to provide evidence for Revalidation and for doctors in training this should be through NHS Appraisal for Doctors in Training, which incorporates College and Faculty documentation. The collection of evidence should have begun on April 1st, 2003, in preparation for Revalidation. In order to maintain a licence to practise a doctor must take part in Revalidation.
By 2008, a new revalidation system was established in response to concerns raised by the Shipman inquiry, and the inquiries into the conduct of a number of other doctors. In future, doctors are required to demonstrate to the General Medical Council that they are up-to-date, and fit to practice medicine. All doctors are required to provide evidence for Revalidation and for doctors in training this should be through NHS Appraisal for Doctors in Training, which incorporates College and Faculty documentation. The collection of evidence should have begun on April 1st, 2003, in preparation for Revalidation.
The concept and underlying principles of Revalidation were set out in the Chief Medical Officer for Englands consultation document Good doctors, safer patients and adopted in the United Kingdom Governments White Paper on professional regulation, Trust Assurance and Safety The Regulation of Health Professionals in the 21st Century (February 2007).
All doctors are now required by law to hold a licence (GMC licences to practice, November 2009) if they wish to exercise the privileges currently reserved for registered medical practitioners (such as prescribing medication and signing death certificates). A new system called revalidation has also begun that requires doctors to renew their licence to practice every five years. The purpose of this new approach to medical regulation is to give patients a regular assurance that licensed doctors are up to date and fit to practice. The process of revalidation involves two strands: relicensing (confirming that doctors practice in accordance with the General Medical Councils generic standards) and recertification (confirming that doctors on the specialist and GP registers conform with standards appropriate for their specialty of medicine).
In England, the Department of Health has established the NHS Revalidation Support Team, which was formerly the Clinical Governance Support Team, to provide expert professional leadership for the design and delivery of new appraisal arrangements in England. On-line appraisal toolkits are available for use by GPs, consultants and staff and associate specialist grade doctors in the NHS. The toolkits can be found at www.appraisals.nhs.uk.
The Appraisal Toolkit is based on the principle that a single portal is available to appraising and appraisee GPs, Consultants and Staff Grade and Associate Specialist (SAS / NCCG) doctors in the NHS in England. This on-line resource brings together advice, guidance, best practice, practical tools and access to a community of peers in the appraisal domain. Detailed guidance on the appraisal process is also provided by the NHS Clinical Governance Support Team, http://www.appraisalsupport.nhs.uk/
References
- Darzi, A. (2008) High Quality Care For All: NHS Next Stage Review Final Report London: Crown
- Department of Health (2008a) Developing the NHS Performance Regime NHS Finance: Performance & Operations
- Department of Health (2008b) Medical Revalidation Principles and Next Steps London: DH Workforce Directorate
- Department of Health (2009) NHS Performance Framework: Implementation guidance Crown http://www.dh.gov.uk/prod_consum_dh/groups/
- Donaldson, L.J. (2001) Professional accountability in a changing world Postgraduate Medical Journal 77:65-67 The Fellowship of Postgraduate Medicine.
- Leatherman, S. and Sutherland, K. (2008) The Quest for Quality: Refining the NHS Reforms. Nuffield Trust
- McSherry, R. and Pearce, P (2002) Clinical Governance A guide to implementation for healthcare professionals Oxford: Blackwell Science
- Pringle, M (2000) Clinical governance in primary care Participating in clinical governance British Medical Journal 321:737-740
- Pencheon, D.; Guest, C.; Melzer, D.; and Gray, M.J.A. (2006) Oxford Handbook of Public Health Practice Oxford University Press.
© S Markwell 2009
