Equality, Equity and Policy: Health and Social Effects of Migration
Migration
Migration is the permanent relocation of an individual from one country to another. The number of international migrants has increased rapidly over recent years, reaching 244 million in 2015. (UN Department of Economic and Social Affairs) There are a variety of different reasons for migration, and migration is often split into two categories - voluntary migration and forced migration. However, some reasons for migration apply to both voluntary and forced migrants, therefore it is more useful to think of reasons for migration in two categories: ‘push’ and ‘pull’ (see Table 1). Push factors drive a migrant out of their country of origin while pull factors attract migrants towards a particular destination country.
Table 1: Push and pull factors
|
Push Factors |
Pull Factors |
|
|
Migrants are a diverse group (e.g. economic migrants, students, refugees, asylum seekers) and therefore the relationship between health and migration is complex. On the one hand, there is a social selection involved in migration (known as the ‘healthy migrant’ effect), since migrants are often younger and healthier compared to both their population of origin and people from the host country of a similar ethnicity. Most evidence of the healthy migrant effect comes from North America, where researchers have found that migrants have a health advantage, which diminishes as individuals become more assimilated into the host society. On the other hand, the migration process may involve a number of stressors and strains that may increase migrants’ morbidity in several ways (figure 1).
Figure 1: The influence of the migration process on migrant’s morbidity.
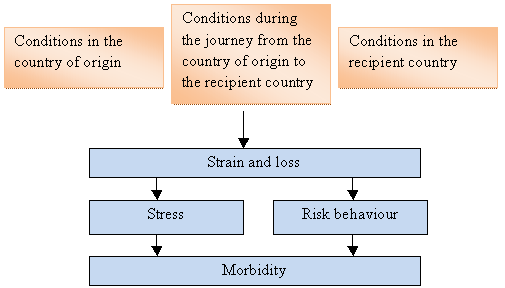
Source: Kristiansen et al, 2007
Conditions affecting health in the country of origin and during the journey may include war, torture, loss of relatives, long stays in refugee camps (which may have poor sanitation and overcrowding), imprisonment, and socioeconomic hardship. After arriving in the host country migrants may experience imprisonment, long-lasting asylum seeking processes, language barriers, lack of knowledge about health services, loss of social status, discrimination and marginalisation.
Kristiansen and colleagues (2007) note that coping with a new language, as well as a new political and social context can be extremely stressful. The effect of migration on the mental health of individuals depends on the magnitude of strains in the recipient country and can be mediated by the migrant’s social resources (i.e. social networks, language skills, education level, etc.).
Migration may also affect risk perception and risk behaviour. Feelings of loss and psycho-social issues related to lower social positions, unemployment and being in a minority may lead to a feeling of lack of connection between current risk behaviour and future health effects (i.e. migrants may be forced to focus on their current feelings rather than the future health effects of their current health behaviour). For example, a new migrant, separated from friends and family in an urban environment (feeling more anonymous and less constrained by social norms) may turn to prostitution or drugs as a way to escape loneliness, frustration and social isolation.
Migration also has health implications for the country migrants have left. Individuals who emigrate for economic opportunities may cause a ‘brain drain’ in their country of origin, when a large number of individuals with technical skills or knowledge leave, potentially depleting the local infrastructure. This particularly affects healthcare because there are often economic incentives for healthcare professionals to migrate. The World Health Organisation (WHO) has long recognised that migration of health personnel from developing to developed countries increases the existing imbalances in the global health workforce and can cause deficiencies in local provision of services in developing countries (Mejia et al, 1979). This migration is often demand-led when developed countries experience shortages in medical professionals. Hagopian et al (2004) estimate that 23% of American physicians received their medical training outside the USA. The majority of foreign trained physicians (64%) in the USA came from middle or low-income countries. In the UK, 31% of doctors and 13% of nurses were born overseas (Glover et al, 2001). While countries of origin may benefit from some remittances (e.g. migrant’s wages sent back), the adverse implications for developing countries greatly outweigh these relatively small benefits. To address the problem of brain drain, Pang and colleagues (2002) recommend “a global perspective, agreed ethical principles between countries, and a systematic approach using the convening power of international organisations.”
Finally, there are health implications of migration in the host (destination) country. Some host countries are worried about the presence of infectious diseases in migrants, and screening of migrants (though a contentious human rights issue) has been adopted, to varying degrees, by several countries throughout the world (Patterson, 2003). While some migrants may be generally healthier than the population (i.e. the ‘healthy migrant’ effect), other migrants may have pre-existing health conditions that can strain local health care systems. For example, increasing retirement migration (where older adults, who often require more health care, migrate to warmer destinations - e.g. Spain, Florida), can present a challenge for recipient health care systems.
References
- Kristiansen M, Mygind A, Krasnik, A (2007). “Health effects of migration”.Danish Medical Bulletin 2007;54:46-7.
- Glover S, Gott C, Loizillon A. Portes J, Price R, Spencer S, Srinivasan V, Willis C (2001). Migration: an economic and social analysis. RDS Occasional Paper No 67, London: Home Office.
- Hagopian A, Thompson M, Fordyce M, Johnson K, Hart LG (2004). “The migration of physicians from sub-Saharan Africa to the United States of America: measures of the African brain drain”. Human Resources for Health, 2:17-26.
- Mejia A, Pizurki H, Royston E: Physician and nurse migration: analysis and policy implications. France, World Health Organisation; 1979:xiii-476.
- Pang T (2002). “Brain drain and health professionals: a global problem needs global solutions”. BMJ, 324:499-500.
- United Nations Department of Economic and Social Affairs Population Division. International Migration Report 2015: Highlights. http://www.un.org/en/development/desa/population/migration/publications/migrationreport/docs/MigrationReport2015_Highlights.pdf
- Patterson R (2003). “Screening immigrants for infectious diseases.” The Lancet Infectious Diseases, 3(11):681
© Rebecca Steinbach 2009, Margaret Eni-Olotu 2016
