PLEASE NOTE:
We are currently in the process of updating this chapter and we appreciate your patience whilst this is being completed.
Concepts of Health and Illness: Activity 4
|
Activity 4: The Effectiveness of Biomedicine in the care of infectious diseases |
From the data set out in the two figures below, what can you deduce concerning the factors responsible for the significant reduction in deaths from Respiratory Tuberculosis and Whooping Cough over the course of the 19th and 20th centuries ?
Respiratory Tuberculosis
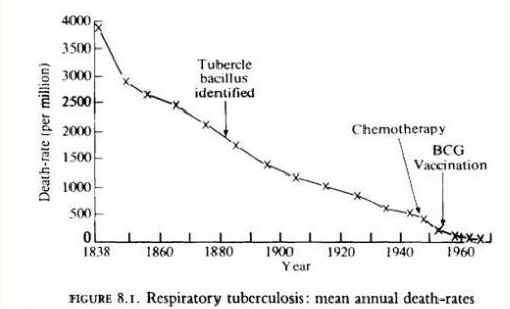
Whooping Cough
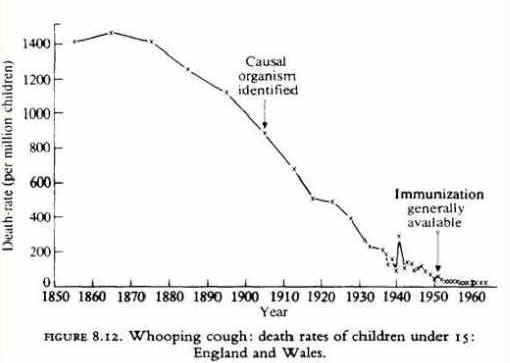
© I Crinson 2007
