Principles and Practice of Health Promotion: Health Promotion and Intersectoral Working
This section covers:
- The role of target-setting eg Public Service Agreements, Local Authority Agreements
- The role of legislative, fiscal and other social policy measures in the promotion of health
- Partnerships
- The benefits and means of community development, including the roles and cultures of partner organisations such as local authorities
- The role of strategic partnerships and the added value of organisations working together
Introduction
This section will review the history of policy development in England that has emphasised the necessity to work in partnership across agencies, and provide some examples of current practice and lessons learnt. Similar policy and practice initiatives apply to other parts of the UK. Partnerships are important because they enable action on the determinants of health, which is vital in order to address health inequalities. Learning from research on building better partnerships to develop more effective and sustainable partnerships is also explored.
The origins of partnership working go back to the emphasis on intersectoral action in WHO Health for All by the Year 2000 (WHO,1981,1985), in particular target 13 which stated that by 1990: 'national policies in all member states should ensure that legislative, administrative and economic mechanisms provide broad intersectoral support and resource for the promotion of healthy lifestyles…' The WHO Healthy Cities Project aimed to put health on the agenda of decision-makers in cities in Europe by applying HFA strategy at city level as a test bed for intersectoral planning and policy-making. This project started with eleven official cities in 1987 but the movement caught on and by 1990 some four hundred cities around the world were attempting to develop a 'healthy city' approach. This was also happening in the UK, not only at city level, but in health and local authorities around the country.
4.1 Intersectoral policy and development of partnership work
In England this was acknowledged in the 1992 government health strategy, 'The Health of the Nation' (DOH, 1992) which first used the term 'healthy alliances' in policy to describe joint working between health and local government for health promotion; 'Healthy alliances…add significantly to the opportunities for progress towards the national targets…achievement of the targets will be enhanced if action - above all joint action - is pursued in the places where people live and work.'
While Health of the Nation supported a settings-based approach to health promotion, and focussed on partnership working as a means of achieving the national health targets, it was strongly focussed on changing health behaviours. As such there was no emphasis on inequalities in health and how to address them. At best these were referred to as health variations, caused by gender, ethnicity etc rather than social and economic determinants. For these reasons this health strategy was widely criticised, although its endorsement of partnership work was a significant step forward.
By 1999 the government produced its revised health strategy for England, 'Our Healthier Nation' (DOH, 1999). This had a much stronger emphasis on health inequality, and also on sharing the responsibility for health improvement across sectors between health and local authorities: 'Tackling poor health and health inequality needs the NHS and local government to take joint responsibility…Successful partnership working is built on organisations moving together to address common goals…'. The focus on inequalities in health was strengthened by the Independent Inquiry into Inequalities in Health - the Acheson Report (1998) which concluded that all policies likely to impact on health should be evaluated in terms of their impact on health inequality; that a high priority should be given in service provision to improve the health of families and children; and that income inequality should be reduced and the living standards of the poor increased. The government response to this in 1999 was to increase the level of income benefits and introduce a minimum wage; to focus on early child development through providing Sure Start preschool services in disadvantaged areas; to establish welfare to work schemes to strengthen employment, and building healthy communities through the creation of Health Action Zones. These initiatives represented a significant cross-sectoral approach to national policy to improve health, particularly amongst the disadvantaged, that would need to be delivered through local partnerships.
By 2001 new national targets were introduced which all public services have to deliver on. These are:
-
by 2010 to reduce inequalities in health outcomes by 10% as measured by infant mortality and life expectancy at birth.
The PSA target is underpinned by two more detailed objectives:
-
starting with children under one year, by 2010 to reduce by at least 10% the gap in mortality between routine and manual groups and the population as a whole.
-
starting with local authorities, by 2010 to reduce by at least 10% the gap between the fifth of areas with the lowest life expectancy at birth and the population as a whole.
In support of these targets there was a cross-cutting review of actions to reduce health inequality across all government departments resulting in a cross government action plan, 'A Programme for Action' (DH, 2003) which had four main themes: supporting families, mothers and children; engaging communities and individuals; preventing illness and providing effective treatment and care, and addressing the underlying determinants of health. In 2004 the partnership approach was re-emphasised in the public health policy Choosing Health (DH, 2004) which states that, 'health needs are complex and real lives do not fit neatly into the boundaries of individual organisations or government departments..'. In addition Choosing Health extends the principle of partnership working to include advertisers, industry and retailers, the employers and the media.
Health inequalities were also a major focus of the UK presidency of the EU in 2005. To emphasise the importance of addressing inequalities in health through intersectoral action, the WHO has also recently established a Global Commission on Social Determinants of Health. As the health sector cannot achieve reductions in inequalities alone, WHP aims to encourage action on the determinants of health globally, through all sectors.
4.2 National intersectoral health promotion programmes
In order to explore how the UK policies and targets have been put into practice, some of the initiatives that have been set up that are predicated upon partnership working between health services and other sectors will be looked at more closely. These are Health Action Zones (HAZs), Sure Start, the National Healthy School Standard (NHSS), and Local Strategic Partnerships (LSPs).
Health Action Zones
Initially 26 Health Action Zones were set up as seven year long pilots in 1997. They aimed to explore mechanisms for breaking through current organisational boundaries to tackle inequalities and deliver better services. Many of these built upon existing healthy alliances that had been following the healthy city model for some years, and had established mechanisms, relationships and procedures in place to focus on joint action to tackle health issues. They have been extensively evaluated and some of their achievements have included:
-
pushing health inequalities up the local agenda by raising the profile of issues and vulnerable groups;
-
broadening the understanding of the determinants of health and of ownership of issues from partners;
-
developing partnership structures and collaborative working;
-
developing more systematic joint planning processes;
-
improving mainstream services especially in disadvantaged areas (Bauld & Judge, 2002).
SureStart
Sure Start is a nationwide initiative that has established community-based programmes in deprived areas to provide services for pre-school children and their families. Their aim is to improve the health and well-being of families with children aged under 4 years, particularly those who are disadvantaged, in order to improve their life chances when they start school. They are based around partnerships of statutory and voluntary agencies, parents and other community members. Each new programme covers a locality with about 400-600 children aged under 4. The SureStart programme is the cornerstone of the UK government's drive to tackle child poverty and social exclusion and thereby improve health, and there has been substantial new investment in these and joined up child health services. They are also subject to extensive evaluation and early findings have suggested that the quality of the partnership working is one of the most significant factors in their successful implementation.
National Health Promoting Schools Programme
There have been active programmes to develop health-promoting schools around the UK for a number of years, that have been supported by local health and education authority alliances. In 1999 the National Healthy School Standard (NHSS) was set up for England to unify these diverse programmes, set common standards and provide national support to local co-ordinators and teachers (www.wiredforhealth.gov.uk). The first phase of the NHSS entailed the accreditation of all the health and education authority partnerships to cover every part of the country, which was completed by 2003. The importance of this phase was to provide a solid foundation of partnership work for further development of schemes to reach as many schools as possible. The second phase put a closer focus on schools in deprived areas, while retaining universal coverage of the scheme. By March 2004 some 10,000 schools were actively engaged in the NHSS in England. Recently government policy has recognised the importance of the education sector to health, and of health to educational attainment, by requiring all schools to become healthy schools by 2009 (DfES, 2004). The ongoing success of health promoting schools has built upon the solid foundations of the partnerships developed, and the continuing engagement of both sectors at local level in schools. (See also Section 3.2 on health promoting settings.)
Local Strategic Partnerships
Local Strategic Partnerships (LSPs) provide another example of the way in which partnerships between the NHS and the local government system in England have been developed to a point where both policy and delivery systems have been integrated at local level. LSPs bring together health, local authority and other bodies in an overarching framework to integrate strategy and service provision. They aim to help core public services to achieve their individual targets for deprived areas via joint working, as well as set up joint targets by helping services to work with each other, with communities and with the private and voluntary sectors. LSPs aim to simplify some of the complexities of current planning and partnership arrangements. They are voluntary partnerships, but the Local Government Act of 2000 has allowed pooling of resources across sectors, which is a major tool to enable the LSP to tackle local priorities. Good leadership is essential, inspiring vision, enthusiasm and commitment, and to command the trust of other partners including local communities. Their core tasks are to:
-
prepare and implement a community strategy for the area;
-
bring together local plans, existing partnerships and initiatives to provide a forum through which mainstream service providers can work effectively to meet local needs and priorities;
-
develop targets and indicators for public service agreements and,
-
a local neighbourhood renewal strategy to secure more jobs, better education, improved health, reduced crime and better housing.
This will lead to closing the gap between deprived neighbourhoods and the rest and contribute to the national inequalities targets. However this is by no means a simple task. The landscape of local partnerships is becoming increasingly complex and it is a major task to connect the many existing topic or issue focussed partnerships and initiatives at local level that are driven by different government policies, (see example in Fig 4.1)
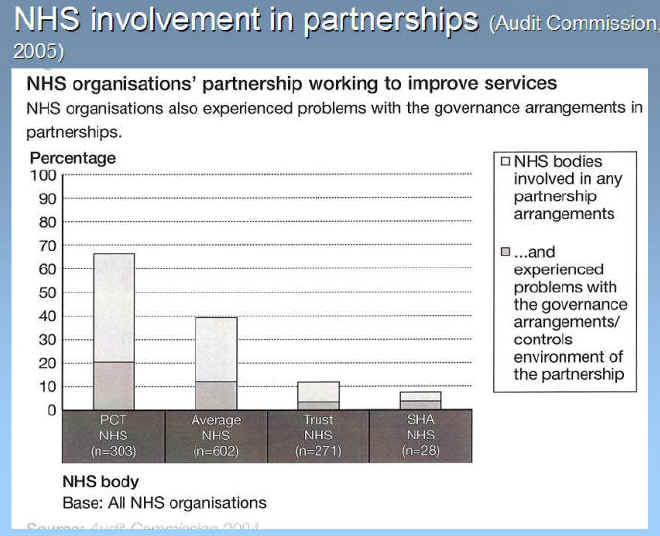
A recent review of LSPs and the lessons about governance learnt has been published by the Audit Commission (2005). This has shown that partnerships are now a significant feature of public service delivery in the UK with over 5500 partnerships accounting for more than £4bn of public expenditure. Funding for partnerships has increased significantly over the last five years with initiatives such as neighbourhood renewal and Sure Start. Almost all local authorities are involved in partnerships and much of the health service, most NHS involvement is through primary care trusts while hospital services are rarely actively involved in LSPs, (Figs 4.2 & 4.3) However up to a quarter of bodies reported that they have experienced problems with governance or accountability controls. The key findings of the Audit Commission's review were that partnerships bring significant benefits and are a response to the complex and multifaceted problems that cannot be tackled by any individual body working alone. However they also bring risks, as working across organisational boundaries brings complexity and ambiguity. It is necessary for organisations to be clear about what they trying to achieve, and whether a partnership is the best way to tackle an issue. Experience of partnership working, and the skills and attitudes required to make it successful takes time to develop. It is evident that the most successful partnerships have built upon a long history of collaboration. Governance and accountability mechanisms need to be clear for them to be successful, and this is helped by use of processes such as partnership agreements, pooled budgets and formalised Local Area Agreements about specific service delivery. In addition, clarity is also needed from central government about the roles and relationships of different partnerships. Often, central policy directives do not take account of the difficulties of integration of different priorities locally.
Figure 4.1 The complexity of partnership working (Audit Commission, 2005)
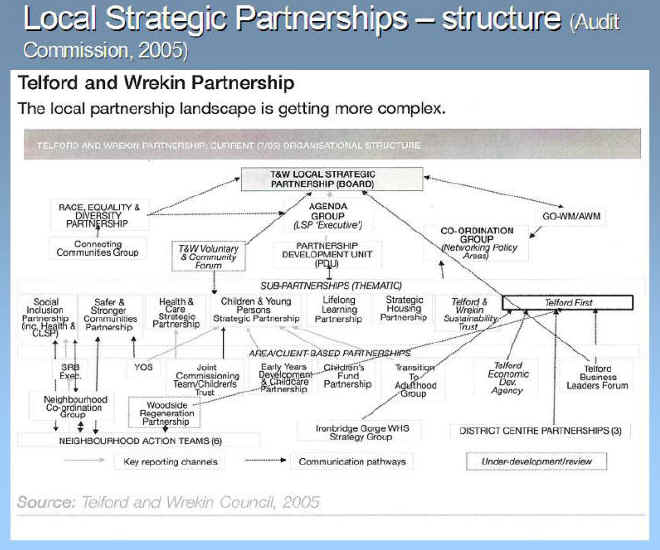
Figure 4.2 Local authority involvement in partnerships (Audit Commission, 2005)
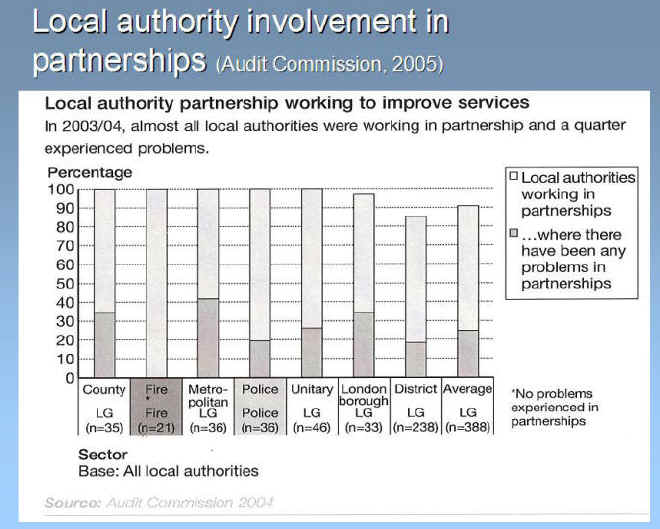
Figure 4.3 NHS involvement in partnerships (Audit Commission, 2005)
Local Area Agreements
Local Area Agreements (LAAs) are an opportunity for LSPs to demonstrate that they have the capacity to add value by helping to bring about improved performance in shared outcomes. LAAs also represent a significant opportunity for LSPs to exert a more effective governance role, enhancing their role as the forum within which partners come together to agree and deliver on local priorities, and enabling them more effectively to influence the mainstream policies of partner agencies. But LAAs also represent a major challenge to local partnership working. Many LSPs lack the capacity and structures for rapid and effective decision-making which the LAAs will require. LAAs may highlight tensions between efficient decision making and wide participation, and weaknesses in communication channels. The LAA process is particularly challenging for county level partnerships, where the number of stakeholders is potentially very large and there may be intra-sector tensions to be resolved, and for sectors which lack responsive decision making structures. LAAs also require some mechanism for focused work and decision making within each of the blocks, and effective links between the LSP and the sub-partnerships that are likely to be best placed to fulfil this role. Furthermore, LAAs potentially represent a radical shift in the relationships between LSPs and government, with the Government Offices' performance management, support and intervention role - hitherto confined to LSPs in NRF areas - being extended to all LSPs. The national evaluation of LSPs (ODPM, 2006) has shown that in the areas of creating a combined vision, strategy and plans, ie process rationalization, there has been good progress. However, there has been less measurable impact and little progress on the structural rationalization of the complexity and layers of partnership structures.
Taking the process of 'engendering systematic partnership working between the NHS, local authorities and other bodies' further in order to make partnership working 'a normal way to do business' (Dept. for Communities and Local Government, 2006), the Local Government White Paper Strong and Prosperous Communities sets out a new policy framework learning from the experience and evaluations of LSPs and LAAs , and aligning local government policy with health policy in Our Health, Our Care, Our Say (DH, 2006). There will be a new requirement to align the services provided by a number of agencies, while local authorities are already under a duty to prepare a Sustainable Community Strategy - which sets a strategic vision for the area, now all County and Unitary authorities, in consultation with partners, will have to prepare a delivery plan for the strategy, ie an LAA. There will be a single set of targets tailored to local need and a simplification of the current performance management framework. In addition there is a proposal to legislate for a new statutory partnership for Health and Well-Being under the LSP. While many LSPs will already have such an arrangement this will make it a requirement of all. It will propose a new duty to co-operate with the PCTs in order to enable local partners to achieve a truly integrated approach to the delivery of local government and NHS priorities. In addition there will be an emphasis on a greater use of joint appointments, including the Director of Public Health, pooled budgets and joint commissioning (DCLG, 2006).
4.3 Effective partnership working
Partnerships don't just happen; and, as the Audit Commission report has shown, they don't always run smoothly. Despite the policy changes over recent years few workers at any level have had a great depth of experience in multi-sectoral working. It brings its own challenges of understanding others' points of view, compromise and conflict resolution. Most people in work are trained in a single discipline in an agency and adopt the norms and mores of that sector. Although recent trainees may have had more multi-disciplinary experience; national policy and resourcing has traditionally come down to local level in vertical streams. This makes it hard for workers to be flexible with their use of budgets, or having to assess their performance in contradictory ways. The more joined up healthy public policy is at national level, as demonstrated by the intentions of Strong and Prosperous Communities, the easier it is for partnerships to be innovative, responsive to local need and deploy resources accordingly. In reality, partnership working is the skill of juggling information and priorities to get the best match of service delivery with health need across sectors, which requires excellent leadership and different approaches to working at all levels.
Experience of working in partnerships has demonstrated that there are key factors or characteristics that make a partnership effective. Different kinds of partnerships will be effective under different conditions, according to local needs and circumstances, but there are factors that are common to all successful partnerships. A growing body of evidence from inter-agency and collaborative practice has led to improved understanding of the factors that make partnerships more effective. Analysis of effective partnership working (Audit Commission, 1998; Pratt et al, 1998) shows that these factors are centred on the following elements:
-
Leadership and vision - the management and development of a shared, realistic vision for the partnership's work through the creation of common goals. Effective leadership is demonstrated by influencing, communicating with and motivating others, so that responsibility for decision-making is shared between partners.
-
Organisation and involvement - the participation of all key local players, and particularly the involvement of communities as equal partners. Not everyone can make the same contribution. Most voluntary organisations are small and locally based, with few staff. They may need resources and time to enable them to become fully engaged.
-
Strategy development and co-ordination - the development of a clear, community focussed strategy covering the full range of issues supported by relevant policies, plans, objectives, targets, delivery mechanisms and processes. Development of local priorities for action will rely on the assessment of local needs, sharing of data, and a continuing dialogue between partners.
-
Learning and development - effective partnerships will not only invest in shared objectives and joint outcomes, but will also add value through secondments and other opportunities to share learning and contribute to professional and organisational development in partner organisations. Willingness to listen and learn from each other builds trust.
-
Resources - the contribution and shared utilisation of information, financial, human and technical resources. The new freedoms to pool budgets and to provide integrated services for example between NHS primary care and local authority services, can remove some of the traditional barriers to joint working.
-
Evaluation and review - assessing the quality of the partnership process and measuring progress towards meeting objectives. Partnerships need to demonstrate that they are making a difference and that meetings are more than just talking shops. They must also be able to show that they are making real improvements to services.
Partnerships must also devise effective cross-organisational arrangements that can cope with multiple lines of accountability to produce genuine collaborative working. They also need to generate meaningful yet realistic targets for change, and to demonstrate achievements and improvements.
These are formidable challenges that will require long-term commitment. There are a number of barriers to overcome in getting a range of agencies and groups with different responsibilities, structures, systems and cultures to collaborate. Some partnerships, particularly those with a history of working together, may find it easier than others to develop a sustained partnership capable of addressing some of these more complex, longer-term issues. Sustained partnerships take time and demand considerable skills from individuals and organisations. It is one thing to determine policy to set up partnerships to join things up, and quite another to develop the mix of skills, energy and commitment to make partnerships effective.
There are a number of resources and audit tools to support partnership working (Markwell, 2003), the following elements in Box 4.1 are taken from The Working Partnership (Markwell, Watson & Speller et al, 2003), which contains a series of detailed questions for partnership teams to use to assess and improve their ways of working.
|
Box 4.1 Key elements of effective partnership work
Organisation - Clear and effective systems are needed for:
Strategy - The partnership needs to implement its mission and vision via a clear strategy informed by local communities and other stakeholders which focuses on:
Learning - Partner organisations need to attract, manage and develop people to release their full knowledge and potential by:
Resources - The contribution and shared utilisation of resources, including
Programmes - Partners seek to develop coordinated programmes and integrated services that fit together well. This requires attention to:
|
References
- Acheson D (1998) Independent enquiry into inequalities in health: report. London, Stationery Office
- Audit Commission, (1998) A fruitful partnership: effective partnership working. Audit Commission, London
- Audit Commission (2005) Governing partnerships: bridging the accountability gap. www.audit-commission.gov.uk
- Bauld L & Judge K (2002) Learning from Health Action Zones. Aeneas Press
- Information about Sure Start; further information about the national evaluation of Sure Start (NESS) from www.ness.bbk.ac.uk
- Department for Communities and Local Government (2006) Local Government White Paper: Strong and Prosperous Communities, Cm 6939, London, TSO
- Department of Health (1992) The Health of the Nation: a strategy for England. London, HMSO
- Department of Health (1999) Saving Lives: Our Healthier Nation London; The Stationery Office
- Department of Health (2003) Working in partnership to reduce inequalities: A Programme for Action, London, Stationery Office
- Department of Health(2004) Choosing Health - Making healthier choices easier. Cm 6374, London HMSO
- Department of Health (2006) White Paper Our Health, Our Care, Our Say: a new direction for community services. Cm 6767, London, TSO
- Department for Education & Skills (2004) Healthy Living Blueprint for Schools, DfES/0781/2004
- Markwell S (2003) Partnership working: a consumer guide to resources, London, HDA. www.nice.org.uk
- Markwell S, Watson J, Speller V et al (2003) The Working Partnership - Book 1 London, Health Development Agency. www.nice.org.uk
- Office of the Deputy Prime Minister (2006). National evaluation of LSPs: Formative evaluation and action research programme 2002-2005; Final Report. London, ODPM
- Pratt J, Plamping D & Gordon P (1998) Partnership: fit for purpose? King's Fund, London
- World Health Organization (1981) Global strategy for Health for All by the Year 2000, WHO, Geneva;
- World Health Organization (1985) Targets for Health for All WHO Regional Office for Europe, Copenhagen
- World Health Organization (1985) Targets for Health for All, WHO Regional Office for Europe, Copenhagen
- www.wiredforhealth.gov.uk for further information and support materials for schools
© V Speller 2007
